S. Epidermidis Hemolysis On Blood Agar
Muz Play
Apr 05, 2025 · 5 min read
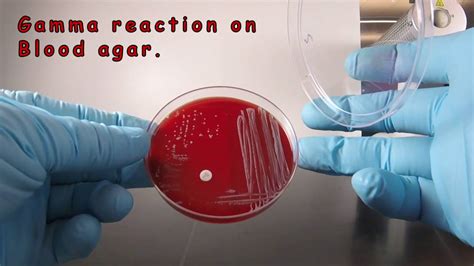
Table of Contents
Staphylococcus epidermidis Hemolysis on Blood Agar: A Comprehensive Overview
Staphylococcus epidermidis, a coagulase-negative staphylococcus (CoNS), is a common inhabitant of human skin and mucous membranes. While generally considered a commensal organism, it can cause opportunistic infections, particularly in immunocompromised individuals or those with implanted medical devices. Understanding its characteristics, including its hemolytic activity on blood agar, is crucial for accurate diagnosis and appropriate management of these infections. This article delves deep into the intricacies of S. epidermidis hemolysis on blood agar, exploring its mechanisms, variations, diagnostic significance, and clinical implications.
Understanding Hemolysis and Blood Agar
Hemolysis refers to the breakdown of red blood cells (RBCs). This process is often observed when bacteria are cultured on blood agar, a rich medium containing 5-10% sheep, horse, or rabbit blood. The type of hemolysis exhibited by a bacterium is a key characteristic used in its identification. Three main types of hemolysis are recognized:
1. Beta-hemolysis (β-hemolysis):
This is characterized by complete lysis of RBCs surrounding the bacterial colony, resulting in a clear, transparent zone around the colony. This indicates the bacterium produces potent hemolysins that completely destroy RBCs.
2. Alpha-hemolysis (α-hemolysis):
This involves partial lysis of RBCs, resulting in a greenish discoloration around the colony. This partial breakdown is usually due to the production of hydrogen peroxide by the bacteria, which oxidizes hemoglobin.
3. Gamma-hemolysis (γ-hemolysis):
This is the absence of hemolysis. There is no change in the appearance of the blood agar surrounding the colony. This means the bacterium does not produce hemolysins.
Hemolytic Pattern of Staphylococcus epidermidis
S. epidermidis is typically described as non-hemolytic or exhibiting weak or no hemolysis (gamma-hemolysis) on blood agar. This means colonies often show no discernible change in the surrounding agar. However, there are exceptions and variations that need to be considered.
Factors Influencing Hemolysis:
Several factors can influence the hemolytic activity of S. epidermidis, making consistent observation challenging. These include:
-
Strain Variation: Different strains of S. epidermidis may exhibit varying degrees of hemolytic activity, with some showing weak alpha-hemolysis, while others remain completely non-hemolytic. This genetic diversity underlines the complexity of interpreting hemolytic patterns.
-
Culture Conditions: Incubation temperature, time, and the type of blood agar used can significantly influence the observed hemolysis. Optimal conditions may be necessary to elicit even weak hemolytic activity.
-
Hemolysin Production: The production of hemolysins, the enzymes responsible for RBC lysis, is not consistently expressed by all S. epidermidis strains. Factors like growth phase and environmental conditions may modulate hemolysin expression.
-
Age of the Culture: The hemolytic activity might change over time as the bacterial culture ages. Older cultures may exhibit less hemolysis than younger ones.
Diagnostic Significance of Hemolysis in S. epidermidis Identification
While the absence of hemolysis is a common feature, it is not solely diagnostic for S. epidermidis. Many other CoNS also exhibit similar patterns. Therefore, relying solely on hemolytic activity to identify S. epidermidis is unreliable. Hemolysis should be considered along with other diagnostic tests for accurate identification.
Other Diagnostic Tests:
Accurate identification of S. epidermidis requires a combination of tests, including:
- Gram staining: Reveals the characteristic gram-positive cocci in clusters.
- Coagulase test: Negative for coagulase, a key differentiating feature from Staphylococcus aureus.
- Catalase test: Positive for catalase, an enzyme that breaks down hydrogen peroxide.
- Biochemical tests: Various biochemical tests help further differentiate S. epidermidis from other CoNS.
- Molecular techniques: Techniques like 16S rRNA sequencing provide definitive identification.
Clinical Implications of S. epidermidis Infections
Although often considered a commensal, S. epidermidis can cause significant infections, particularly in susceptible individuals. Its ability to form biofilms on medical devices is a major factor contributing to its pathogenicity.
Biofilm Formation:
S. epidermidis excels at forming biofilms, which are complex communities of bacteria encased in a self-produced extracellular matrix. Biofilms provide protection from the host's immune system and antibiotics, making infections difficult to treat. These biofilms are commonly associated with infections of:
- Implanted medical devices: Catheters, prosthetic joints, heart valves.
- Surgical wounds: Especially in cases of contaminated surgical sites.
- Other infections: Endocarditis, meningitis (rarely), bacteremia.
Treatment of S. epidermidis Infections:
Treatment of S. epidermidis infections is often challenging due to its biofilm formation and potential antibiotic resistance. Treatment strategies include:
- Antibiotic therapy: Appropriate antibiotics need to be chosen based on susceptibility testing. However, resistance to commonly used antibiotics is a growing concern.
- Device removal: In cases of device-related infections, removing the infected device is often crucial for successful treatment.
- Biofilm disruption: Strategies aimed at disrupting the biofilm structure may enhance antibiotic efficacy.
Research on S. epidermidis Hemolysis and Virulence
While S. epidermidis is often non-hemolytic, ongoing research continues to investigate potential links between hemolytic activity, biofilm formation, and virulence. Some studies suggest certain hemolysins may play a role in the bacteria’s ability to colonize and cause infections. Understanding these mechanisms is crucial for developing improved diagnostic and treatment strategies.
Future Directions:
Future research is crucial in this field. We need a better understanding of:
- The genetic regulation of hemolysin production: This would provide insights into the factors influencing the variable expression of hemolysins.
- The role of hemolysins in biofilm formation: Research could focus on the contribution of hemolysins to biofilm architecture and resistance to host defenses.
- The development of novel diagnostic tools: This involves exploring faster and more precise methods for identifying S. epidermidis and assessing its virulence potential.
- The identification of new therapeutic targets: This is important for developing effective strategies to treat S. epidermidis infections, especially those associated with biofilms.
Conclusion
Staphylococcus epidermidis hemolysis on blood agar is a complex phenomenon with variable expression. While typically non-hemolytic or showing weak alpha-hemolysis, this characteristic alone is insufficient for definitive identification. Accurate diagnosis requires combining hemolysis observation with other microbiological tests. Understanding the role of hemolysins in S. epidermidis pathogenesis, especially in relation to biofilm formation, is crucial for improving prevention and treatment strategies for infections caused by this opportunistic pathogen. Further research is necessary to unravel the complexities of this bacterium and develop targeted approaches to manage the infections it causes. The emphasis should always be on accurate identification through a comprehensive approach rather than relying on a single, potentially variable characteristic like hemolysis.
Latest Posts
Latest Posts
-
What Does It Mean For A Solution To Be Saturated
Apr 06, 2025
-
Describe The Region Enclosed By The Circle In Polar Coordinates
Apr 06, 2025
-
Does Atomic Radius Increase From Left To Right
Apr 06, 2025
-
Molecular Orbital Diagram For H2 And Bond Order
Apr 06, 2025
-
Formulas With Polyatomic Ions Worksheet Answers
Apr 06, 2025
Related Post
Thank you for visiting our website which covers about S. Epidermidis Hemolysis On Blood Agar . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
