Select The Five Major Mechanisms Of Antimicrobial Resistance
Muz Play
Apr 02, 2025 · 6 min read
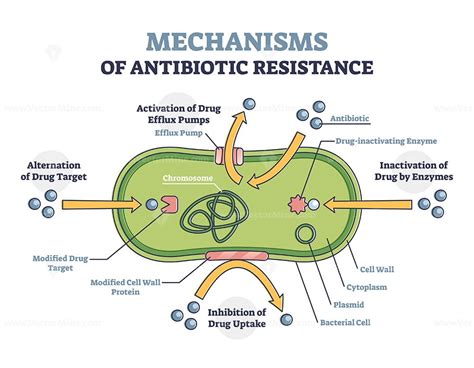
Table of Contents
The Five Major Mechanisms of Antimicrobial Resistance: A Deep Dive
Antimicrobial resistance (AMR) is a global crisis, threatening our ability to treat common infections with antibiotics, antifungals, antivirals, and antiparasitics. Understanding the mechanisms behind this resistance is crucial for developing strategies to combat it. This article delves into the five major mechanisms of antimicrobial resistance, exploring their intricacies and the implications for global health. We will examine how these mechanisms work, the types of microbes they affect, and the challenges they present to healthcare professionals worldwide.
1. Target Modification: Changing the Lock
One primary mechanism of AMR involves altering the drug's target site within the microbe. This is akin to changing the lock on a door so the key (antimicrobial) no longer fits. These modifications can be subtle or substantial, rendering the drug ineffective.
Examples of Target Modification:
- Mutations in ribosomal proteins: Many antibiotics target bacterial ribosomes, the protein synthesis machinery. Mutations in ribosomal proteins can prevent antibiotic binding, reducing the drug's efficacy. This is common in resistance to aminoglycosides and macrolides.
- Changes in penicillin-binding proteins (PBPs): Beta-lactam antibiotics, such as penicillin and cephalosporins, target PBPs involved in bacterial cell wall synthesis. Mutations in PBPs can reduce the antibiotic's affinity for the target, leading to resistance. This is a key mechanism in methicillin-resistant Staphylococcus aureus (MRSA) and penicillin-resistant Streptococcus pneumoniae.
- Alterations in DNA gyrase and topoisomerase IV: Quinolone antibiotics inhibit DNA gyrase and topoisomerase IV, enzymes essential for DNA replication in bacteria. Mutations in these enzymes can prevent antibiotic binding and lead to resistance, observed commonly in fluoroquinolone-resistant bacteria.
- Amino acid changes in enzyme active sites: Many antibiotics target specific enzymes within bacteria. Mutations resulting in amino acid changes within the active site of these enzymes can reduce or eliminate antibiotic binding, hindering the drug’s ability to function. This is observed in resistance to sulfonamides and trimethoprim.
2. Efflux Pumps: Actively Removing the Threat
Bacteria employ efflux pumps, membrane-bound proteins that actively expel antimicrobial agents from the cell. This is like having a powerful pump that removes the key from the lock before it can engage. These pumps are remarkably versatile, capable of expelling a wide range of antibiotics, thereby conferring multidrug resistance.
Characteristics of Efflux Pumps:
- Specificity: While some efflux pumps are specific to certain classes of antibiotics, many have broad substrate specificity, capable of removing various antimicrobials.
- Energy dependence: Efflux pumps require energy to function, utilizing proton motive force or ATP.
- Regulation: The expression of efflux pumps is often regulated, increasing their production in the presence of antibiotics. This adaptive response enhances the bacterium's survival.
- Contribution to multidrug resistance: The broad specificity and regulation of efflux pumps make them a significant contributor to multidrug resistance in bacteria.
3. Enzyme Inactivation: Neutralizing the Attack
Some bacteria produce enzymes that chemically modify or inactivate antimicrobial agents. This is similar to destroying the key before it can reach the lock. These enzymes are often highly specific, targeting particular classes of antibiotics.
Examples of Enzyme Inactivation:
- Beta-Lactamase production: Many bacteria produce beta-lactamases, enzymes that hydrolyze the beta-lactam ring of penicillin and cephalosporin antibiotics, rendering them inactive. This is a major mechanism of resistance to these widely used antibiotics. Extended-spectrum beta-lactamases (ESBLs) are particularly concerning due to their ability to inactivate a broad range of beta-lactam antibiotics. Carbapenemases, another class of beta-lactamases, inactivate even the last-resort carbapenem antibiotics, posing a severe threat to public health.
- Aminoglycoside-modifying enzymes (AMEs): AMEs add chemical groups (e.g., acetyl, adenyl, phosphoryl) to aminoglycoside antibiotics, modifying their structure and preventing their binding to ribosomal targets. This contributes significantly to aminoglycoside resistance in bacteria.
- Chloramphenicol acetyltransferases (CATs): CATs inactivate chloramphenicol by acetylating it, preventing its interaction with bacterial ribosomes.
4. Target Site Protection: Shielding the Vulnerability
Certain mechanisms protect the antibiotic's target site from access. This is akin to placing a barrier in front of the lock, preventing the key from reaching it. This often involves changes in the bacterial cell wall or membrane, limiting antibiotic penetration.
Examples of Target Site Protection:
- Altered outer membrane permeability in Gram-negative bacteria: Gram-negative bacteria have an outer membrane that acts as a permeability barrier. Changes in the composition or structure of this outer membrane can reduce the entry of antibiotics into the cell. This is a common mechanism of resistance in many Gram-negative bacteria, such as Pseudomonas aeruginosa.
- Changes in porin expression: Porins are channel proteins in the outer membrane of Gram-negative bacteria that allow the passage of molecules. Reduced expression or alteration of porins can limit antibiotic entry.
- Increased efflux pump expression, revisited: While primarily discussed as a separate mechanism, increased expression of efflux pumps can also indirectly protect the target site by removing the antibiotic before it can reach its target.
5. Antibiotic Target Overproduction: Overcoming the Blockade
In some cases, the bacterium simply overproduces the target of the antibiotic. This is analogous to having multiple locks, so even if one is compromised, others remain functional. By increasing the amount of the target protein, the bacterium ensures sufficient functionality despite antibiotic binding to a fraction of the molecules.
Examples of Target Overproduction:
- Increased dihydrofolate reductase production: Trimethoprim targets dihydrofolate reductase, an enzyme essential for folate biosynthesis. Bacteria can develop resistance by overproducing this enzyme, overcoming the inhibitory effect of the drug.
- Increased dihydropteroate synthase production: Sulfonamides inhibit dihydropteroate synthase, another enzyme in folate biosynthesis. Similar to dihydrofolate reductase, bacteria can develop resistance by overproducing this enzyme.
Conclusion: The Complex Landscape of Antimicrobial Resistance
The five major mechanisms of antimicrobial resistance—target modification, efflux pumps, enzyme inactivation, target site protection, and antibiotic target overproduction—are intricately interwoven and often work in combination. Understanding these mechanisms is pivotal in designing new strategies to combat AMR. This requires a multi-pronged approach including:
- Developing new antibiotics targeting novel mechanisms: This necessitates investment in research and development of novel antimicrobial agents that bypass existing resistance mechanisms.
- Improving diagnostics to identify resistance mechanisms: Rapid and accurate detection of resistance mechanisms is critical for guiding appropriate antibiotic treatment and preventing further spread of resistant strains.
- Implementing infection control measures: Strict adherence to infection control protocols in healthcare settings is vital in reducing the spread of resistant microorganisms.
- Promoting judicious antibiotic use: Responsible prescribing and patient adherence to antibiotic treatment guidelines are essential in minimizing the selective pressure that drives the development of AMR.
- Exploring alternative therapeutic strategies: Investigating alternative therapeutic approaches, such as phage therapy, immunotherapies, and novel adjuvants, is crucial in complementing existing antibiotic treatments.
The fight against antimicrobial resistance is a global challenge requiring collaborative efforts from researchers, healthcare professionals, policymakers, and individuals. By understanding the complexities of AMR and implementing evidence-based strategies, we can strive towards a future where infections remain treatable and preventable. The continued exploration and detailed understanding of these five mechanisms will be vital in this critical endeavor.
Latest Posts
Latest Posts
-
Draw A Phasor Diagram Showing Generator Voltage At Time 0
Apr 03, 2025
-
What Is A Wet Mount Slide
Apr 03, 2025
-
Examples Of Stoichiometry In Real Life
Apr 03, 2025
-
Why Is Water Necessary For Biological Organisms
Apr 03, 2025
-
How Is Probability Used In Genetics
Apr 03, 2025
Related Post
Thank you for visiting our website which covers about Select The Five Major Mechanisms Of Antimicrobial Resistance . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
