What Is The Smallest Functional Unit Of The Kidney
Muz Play
Apr 04, 2025 · 7 min read
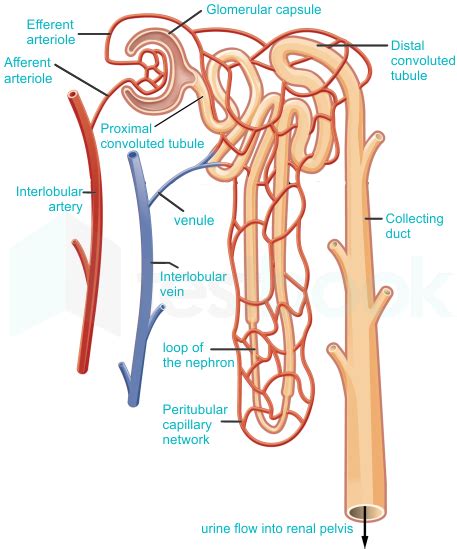
Table of Contents
What is the Smallest Functional Unit of the Kidney? Understanding the Nephron
The kidney, a vital organ in the urinary system, plays a crucial role in maintaining overall health by filtering blood and removing waste products. But what exactly is the smallest unit responsible for this complex process? The answer is the nephron. This intricate structure is the fundamental functional unit of the kidney, responsible for the intricate processes of filtration, reabsorption, and secretion that ultimately lead to urine production. Understanding the nephron's structure and function is key to grasping the complexity and importance of kidney function.
The Structure of the Nephron: A Microscopic Marvel
Each kidney contains approximately one million nephrons, and their combined action ensures efficient waste removal and electrolyte balance. The nephron is not a simple structure; rather, it's a complex network of specialized tubules and associated blood vessels. It can be broadly divided into two main parts:
1. Renal Corpuscle: The Filtration Unit
The renal corpuscle, also known as the Malpighian body, is the initial filtering component of the nephron. It consists of two structures:
-
Glomerulus: This is a network of capillaries where blood filtration begins. The glomerulus is highly specialized; its capillaries are fenestrated, meaning they have pores that allow the passage of water and small solutes but prevent the passage of larger molecules like proteins and blood cells. The high pressure within the glomerular capillaries is crucial for efficient filtration. This pressure is maintained by the afferent arteriole (the artery bringing blood to the glomerulus) having a larger diameter than the efferent arteriole (the artery taking blood away from the glomerulus).
-
Bowman's Capsule: This cup-shaped structure surrounds the glomerulus and collects the filtrate produced. The filtrate, essentially plasma minus proteins and blood cells, is then passed on to the next stage of nephron function. The inner layer of Bowman's capsule consists of specialized cells called podocytes, which further refine the filtration process. Podocytes have intricate finger-like projections called pedicels that interdigitate, leaving narrow filtration slits. These slits act as an additional barrier, preventing larger molecules from entering the filtrate.
2. Renal Tubule: Fine-tuning the Filtrate
The renal tubule is a long, convoluted tube that extends from Bowman's capsule. It's responsible for modifying the filtrate through reabsorption and secretion. The renal tubule can be further subdivided into several segments, each with a unique function:
-
Proximal Convoluted Tubule (PCT): This is the first segment of the renal tubule and is characterized by its highly convoluted structure. The PCT is responsible for the majority of reabsorption in the nephron. Essential nutrients like glucose, amino acids, and water are actively reabsorbed back into the bloodstream, along with vital electrolytes like sodium, potassium, and chloride. The PCT also plays a role in secreting hydrogen ions and other waste products into the filtrate.
-
Loop of Henle: This U-shaped structure extends from the PCT and dips into the renal medulla. The loop of Henle plays a crucial role in establishing a concentration gradient in the renal medulla, essential for concentrating urine. The descending limb is permeable to water but relatively impermeable to solutes, while the ascending limb is impermeable to water but actively transports sodium and chloride ions out of the filtrate. This countercurrent multiplier system creates a hyperosmolar environment in the medulla, facilitating water reabsorption in the collecting duct.
-
Distal Convoluted Tubule (DCT): This segment continues from the loop of Henle and is involved in fine-tuning electrolyte balance. The DCT is influenced by hormones like aldosterone and parathyroid hormone, which regulate sodium and calcium reabsorption, respectively. It also secretes potassium ions and hydrogen ions, contributing to acid-base balance.
-
Collecting Duct: The collecting duct is not strictly part of a single nephron but receives filtrate from multiple nephrons. It plays a critical role in regulating water reabsorption and urine concentration under the influence of antidiuretic hormone (ADH). ADH increases the permeability of the collecting duct to water, allowing for greater water reabsorption and the production of concentrated urine. In the absence of ADH, the collecting duct is less permeable to water, leading to the production of dilute urine.
Nephron Function: A Symphony of Processes
The overall function of the nephron is a coordinated effort of three major processes:
1. Glomerular Filtration: The Initial Sieve
Glomerular filtration is a passive process driven by the hydrostatic pressure difference between the glomerular capillaries and Bowman's capsule. This pressure forces water and small solutes from the blood into Bowman's capsule, forming the filtrate. The filtration membrane, composed of the fenestrated endothelium, basement membrane, and podocytes, acts as a selective filter, preventing large molecules from entering the filtrate.
2. Tubular Reabsorption: Reclaiming the Valuable
Tubular reabsorption is the process by which essential substances filtered into the nephron are reabsorbed back into the bloodstream. This is an active and passive process occurring along the different segments of the renal tubule. Glucose, amino acids, and electrolytes are actively transported back into the peritubular capillaries, while water follows passively by osmosis.
3. Tubular Secretion: Active Removal
Tubular secretion is an active process by which substances are transported from the peritubular capillaries into the renal tubule. This process serves to further remove waste products and regulate the pH of the blood. Hydrogen ions, potassium ions, and certain drugs are secreted into the filtrate, contributing to the removal of metabolic waste and maintaining acid-base homeostasis.
Nephron Types: Juxtamedullary vs. Cortical
While all nephrons perform the same basic functions, they differ slightly in their location within the kidney and the length of their Loop of Henle. This leads to functional differences in their contribution to urine concentration:
-
Cortical Nephrons: These are the most abundant type, located predominantly in the renal cortex, with short Loops of Henle that extend only slightly into the medulla. They primarily contribute to the filtration and reabsorption of water and solutes.
-
Juxtamedullary Nephrons: These nephrons are located close to the corticomedullary junction, with long Loops of Henle that extend deep into the renal medulla. Their long Loops of Henle are crucial for establishing the concentration gradient necessary for producing concentrated urine. This is vital for conserving water in conditions of dehydration.
Clinical Significance of Nephron Function: Diseases and Disorders
Understanding nephron function is critical in diagnosing and treating various kidney diseases. Damage or dysfunction of nephrons can lead to a range of conditions, including:
-
Acute Kidney Injury (AKI): This is a sudden decrease in kidney function, often caused by factors like dehydration, infection, or exposure to nephrotoxic substances. AKI can result in a build-up of waste products in the blood and electrolyte imbalances.
-
Chronic Kidney Disease (CKD): This is a progressive loss of kidney function over time, often due to conditions like diabetes, hypertension, or glomerulonephritis. CKD can eventually lead to end-stage renal disease (ESRD), requiring dialysis or kidney transplantation.
-
Glomerulonephritis: This is a group of diseases characterized by inflammation of the glomeruli, affecting their filtering capacity. Glomerulonephritis can lead to proteinuria (protein in the urine) and hematuria (blood in the urine).
-
Polycystic Kidney Disease (PKD): This is a genetic disorder characterized by the development of cysts in the kidneys, leading to impaired kidney function.
Conclusion: The Nephron – A Foundation of Health
The nephron, as the smallest functional unit of the kidney, plays a pivotal role in maintaining overall health. Its intricate structure and coordinated functions ensure the efficient removal of waste products, regulation of fluid balance, and maintenance of electrolyte homeostasis. Understanding the nephron's structure and function is essential for comprehending the complex physiology of the kidney and appreciating the importance of this vital organ in maintaining overall health. Disruptions to nephron function can have significant clinical consequences, highlighting the importance of protecting kidney health through lifestyle choices and medical interventions. Further research into nephron biology and function continues to provide insights into the development of novel treatments for kidney diseases.
Latest Posts
Latest Posts
-
What Is The Number Of Protons For Sulfur
Apr 04, 2025
-
What Is The Atomic Radius Of Hydrogen
Apr 04, 2025
-
What Are The Two Kinds Of Matter
Apr 04, 2025
-
How Is A Subsatnce Saruaryed On A Graph
Apr 04, 2025
-
Based On The Frequency Distribution Above Is 22 5 A
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about What Is The Smallest Functional Unit Of The Kidney . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
